Chiropractic
Gluteal tendinopathy AKA – Hip bursitis
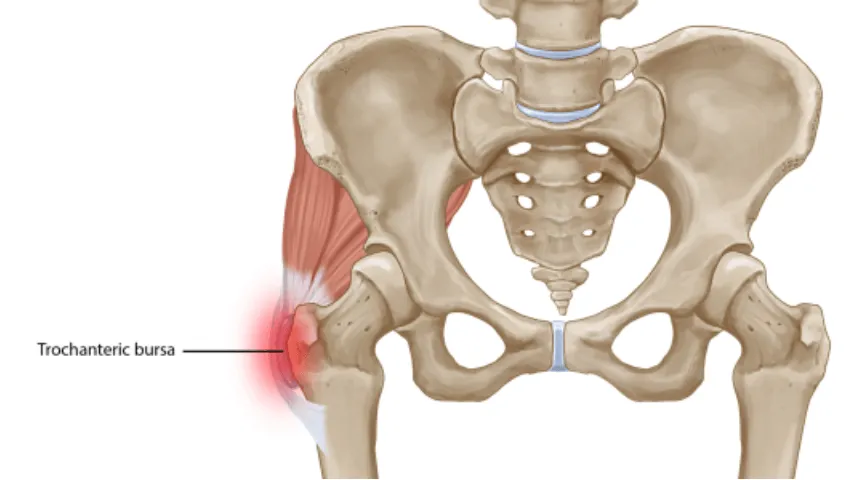
A common injury we see presenting to the clinic is pain on the side of the hips – commonly referred to as hip bursitis over the years. The name has changed over time, from hip bursitis, trochanteric bursitis to now commonly referred to as gluteal tendinopathy. Our understanding of the tissues involved has also evolved, which I will go into further detail below.
Often the most common complaints is that it hurts to sleep on the involved side – and thus causes a lot of interrupted sleep. The bursa that sits on the side of the hip is often blamed, though this is now known to not be the main cause – rather it is a symptom. The main pathology is the tendon of the gluteal muscle – which sits on top of the bursa – it is weak. As a result, the tendon thickens and pain generators are active – causing the tendon to become sensitised.
Gluteal tendinopathy is more common in women than men, especially after menopause. It can also affect people who do activities that involve a lot of running, jumping, or twisting of the hips. Some of the symptoms of gluteal tendinopathy include:
- Pain on the side of your hip that may radiate down your leg
- Difficulty sleeping on the affected side
- Difficulty walking, climbing stairs, or getting in and out of a car
- Reduced range of motion of your hip joint
What causes It?
The main cause is overloading or too much compression of the tendon. This can happen when you:
- Stretch your hip too much or too often – across your midline
- Cross your legs when sitting or lying down
- Stand with your hip tilted to one side
- Wear shoes that are too high or too low
The interesting thing about gluteal tendinopathy is that you can do these things for years and you will have no symptoms. Although there could be a time when the tendon becomes fatigued – often due to an increase in activity over a short period of time and that can flare up the tendon.
How can it be treated?
The first thing we need to do is desensitise the tendon – that is stop irritating it! The number one thing to do is to stop stretching it! A lot of people think stretching the tendon will help, but this just irritates it. The next thing to do is stop the leg from crossing your midline – which means the tendon is not stretched or compressed.
Seeing a chiropractor can help by providing education and also:
- Hands on treatment to mobilise and manipulate your joints and soft tissues
- Exercise prescription to target your gluteal muscles and other supporting structures
- Advice on how to progress your activity level safely and gradually
Gluteal tendinopathy can be a chronic and debilitating condition, but it does not have to be. With proper management and care, you can reduce your pain, improve your function, and enjoy life again.
Call 99975773 to book in to see one of our chiropractors so we can fix your gluteal tendinopathy today!
Mitchell Roberts – Chiropractor
Jaw Pain? Don’t Suffer in Silence!
As a chiropractor, I’ve noticed a significant increase in patients coming to me with jaw pain and discomfort. It’s a problem that often gets overlooked, but it can have a huge impact on your daily life. Everything from eating and talking to sleeping can become a struggle when your jaw isn’t functioning properly. What is TMJ Disorder? TMJ stands for temporomandibular joint, which is the hinge joint that connects your jawbone to your skull.
TMJ disorder is a condition that causes pain and dysfunction in this joint and the surrounding muscles. Symptoms of TMJ Disorder TMJ disorder can manifest in a variety of ways, including:
- Pain or tenderness in your jaw
- Clicking, popping, or grating sounds when you open or close your mouth
- Difficulty chewing or a feeling that your bite is “off”
- Headaches, earaches, or neck pain
- Locking of the jaw joint How I Can Help with TMJ Pain Many people are surprised to learn that chiropractic care can be an effective treatment for TMJ disorder. Here’s how I approach it in my practice:
- Thorough Assessment: I’ll start by asking you about your symptoms, medical history, and any factors that might be contributing to your jaw pain. I’ll also conduct a physical examination of your jaw, neck, and spine.
- Collaboration with Other Professionals: I believe in a team approach to healthcare. I often liaise with your GP and dentist to ensure we’re all working together to address your specific needs. This might involve getting X-rays or other imaging to rule out any underlying dental issues.
- Personalised Treatment Plan: Based on my assessment, I’ll create a customised treatment plan to address the root cause of your TMJ disorder. This may include:
- Gentle Chiropractic Adjustments: To improve the alignment and function of your jaw, neck, and spine.
- Soft Tissue Therapy: To release tension in the muscles surrounding your jaw.
- Targeted Exercises: To strengthen and stabilise your jaw muscles.
- Lifestyle Advice: To help you identify and modify any habits that might be contributing to your jaw pain, such as teeth grinding or clenching.
If you’re experiencing jaw pain or any symptoms of TMJ disorder, I encourage you to schedule an appointment today. With the right care and support, you can find relief and get back to enjoying life without the limitations of jaw pain.
Mitchell Roberts – Chiropractor
Spring 2023 Newsletter
As we bounce into Spring, we focus on the following:
- Tips for gardening safely
- Tina’s tasty treat
- Introducing Zachary
- Pip’s tips for getting a goodnight sleep
- Magnesium and Inflavanoids
Rigid vs Kinesio Taping
Another common question I get asked in clinic is the difference between the two most used taping methods – rigid and kinesio taping. In short, rigid taping is used for joints such as ankles and shoulders to provide added support, while kinesio tape is used for muscles and joints. They work very differently, which I will explain below.
Here at Mona Vale Chiropractic Centre, we use both forms regularly.
Rigid Taping:
Rigid taping is the most common technique and has been used for a very long time in sport. It is used primarily on joints such as ankles, knees, wrists, elbows and shoulders. The role of the tape is to physically support the joint by limiting movement. The tape is primarily used in returning to sport after a joint sprain, for example an ankle sprain. It provides support and stability that gives the athlete confidence within the joint. It is commonly used in rugby union/league, AFL and netball.
Kinesio Taping:
Kinesio taping works entirely different to rigid. The tape is quite stretchy and is applied in a stretched position. Because it is stretched, it bunches once applied. This bunching lifts up the different layers of skin, fascia and muscles which encourages blood flow and lymph drainage within the area.
This tape does not restrict joint movement, rather it increases joint proprioception. This is very effective in rehabilitating post an ankle sprain, as often the joint is weak and feedback from the joint to the brain for positional awareness is reduced. The tape provides a stimulation of the skin that alerts the brain to the area, thus more muscle and joint activation.
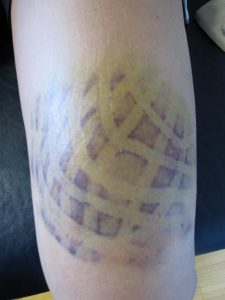
Kinesio taping is also very good at reducing swelling and bruising. As can be seen from the picture below
Another benefit is that kinesio tape can be kept on for 5-6 days post application and can be worn through vigorous training, swimming and showering. Here at Mona Vale Chiropractic Centre we use and recommend Rocktape.
To sum up, both tapes are very effective when applied properly. Contact us at Mona Vale Chiropractic Centre to discuss with us which tape is best suited for your injury
Mitchell Roberts – Chiropractor
Exercising into pain with a chronic injury?
A recent systemic review and meta-analysis titled “Should exercises be painful in the management of chronic musculoskeletal pain?” by Smith et al 2017 was published. It looked at exactly what is mentioned in the title, should it hurt when performing rehabilitation exercises. This is a very common question I get when in clinic and prescribing exercises.
The findings as listed in the paper:
· Protocols using exercises into pain for chronic musculoskeletal pain offer a small but significant benefit over pain free exercises in the short term
· Adults with musculoskeletal pain can achieve significant improvements in patient reported outcomes with varying degrees of pain experiences and post recovery time with therapeutic exercise
· Pain during therapeutic exercise for chronic musculoskeletal pain need not be a barrier to successful outcomes
· Protocols using exercises into pain typically have higher loads and dose of exercise
So the short answer is yes! Exercising into pain is OK if you have a chronic injury.
The theory behind why exercising into pain being beneficial is that it effects the central nervous system. The exercises address psychological factors behind chronic pain, that being fear avoidance behaviours. When we have chronic pain, our movement patterns are different – due to the subconscious mind/nervous system tightening up and restricting/guarding against movements.
Therefore, by moving/exercising into pain, it tells the brain that the tissues are OK and that by progressing it is not causing damage to the tissues. A hurdle that is often hard to overcome in chronic pain is that pain does not equal tissue damage.
Please note, that this research is into chronic musculoskeletal pain (lasting greater than 3 months), not acute pain. Consult with your health care professional before starting an exercise rehabilitation program.
Smith BE, Hendrick P, Smith TO, et al. Should exercises be painful in the management of chronic musculoskeletal pain? A systematic review and meta-analysis
Br J Sports Med Published Online First: 08 June 2017. doi: 10.1136/bjsports-2016-097383
http://bjsm.bmj.com/content/early/2017/07/12/bjsports-2016-097383
Mitchell Roberts – Chiropractor
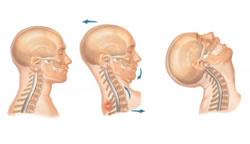
What is whiplash?
Whiplash is a quick, sudden hyperextension and then hyperflexion movement of the neck. The most common cause is a motor vehicle accident, although it also can occur in contact sports and falls.
The sudden movement causes the muscles, tendons and ligaments to be stretched beyond their normal limits, resulting in tissue damage and a generalised pain in the neck, upper back and even sometimes in the lower back. The reason for this generalised pain is that the nervous system is in shock, due to the extreme sudden movement of the neck. Restricted movement results, which is the nervous system protecting the spine from further damage.
Whiplash associated disorder (WAD) is categorised into four stages:
- WAD I – Neck pain with stiffness or tenderness, no physical signs
- WAD II – Neck pain with musculoskeletal signs, such as decrease in range of motion
- WAD III – Neck pain with neurological signs, such as numbness, pins & needles or weakness of the upper limbs
- WAD IV – neck pain with a fracture or dislocation of the neck
The most common presentation to a chiropractor is WAD II.
There is also other symptoms involved with whiplash, which include, but not limited to – headache, arm weakness, jaw pain, dizziness, vertigo and pain when swallowing.
Do the symptoms occur straight away?
Whiplash symptoms do not always occur straight away. There can often be a delay of a few days in which the patient will start to report stiffness and a generalised pain around the upper back and neck.
Is an x-ray or MRI needed?
Imaging depends upon the symptoms. For a WAD I & II, imaging is not often required, as the injury is soft tissue. If a fracture is suspected, an X-ray will be needed. If there are neurological symptoms present, MRI is often needed to see and identify what is causing the symptoms.
Do I need to wear a cervical collar to immobilise?
No! A collar is not recommended, unless there is a fracture suspected or neurological signs present. The best thing for whiplash that is diagnosed as WAD I or II post injury is to encourage gentle movement.
How long does whiplash last for?
The duration of whiplash is quite variable and varies between person to person. Typically, recovery occurs withina few weeks, although it can last for up to 6 months and possibly longer. Receivingappropriate treatment and performing the provided exercises ensures the best outcome.
What is the treatment?
After a thorough history and examination, an individual treatment program will be provided with appropriate manual therapy and rehabilitation exercises to help improve joint range of motion, decrease pain and loosen muscles. Joint manipulation is often used, although not always straight after a whiplash injury.
If we deem that chiropractic treatment is not suitable for your injury, a referral to an appropriate health care provider will be given.
If you are suffering from whiplash, please contact us on at Mona Vale Chiropractic Centre on 99975773 to make an appointment, so we can help you begin your recovery from a whiplash injury.
Mitchell Roberts – Chiropractor
Just how heavy is your child’s school bag?
I often ask parents how heavy their children’s school bag is and the reply almost every time is ‘far too heavy’. A great new research paper has just come out titled “The weight of pupils’ schoolbags in early school age and its influence on body posture”. I will summarise points below and there is also a link to the paper (full text is available) at the bottom of this post.
The study looked at 168 children aged 7-9 over a period of 1 year and looked at school bag weight, length of straps and certain body posture measurements.
- School bag weight ranged between 4.7-9.0kg, with an average weight of 6.3kg. The recommended weight for school bags for students aged between 7-9 should be between 3.1-5.9kg
- More than 90% of the students improperly put on and took off their school bags. This involved a bending motion accompanied by rotation and a rapid straightening of the lumbar spine
- 79.3% had the two shoulder straps adjusted at different lengths
- School bags were most often placed too high, which forced children to lean forward and hence overload the spine
Some general tips for carrying backpacks:
- Backpacks should ideally be no heavier than 10% of the students body weight
- Use both shoulder straps, both of even length. Do not carry it over one shoulder
- Use the waist straps
- Heavy items should be placed at the bottom of the bag and close to the spine
- Lift a backpack through squatting, backpack held close to the body
If you have any concerns about the effects of your child’s backpack on their spinal health, bring them in to see one of the chiropractors here at Mona Vale Chiropractic Centre.
The weight of pupils’ schoolbags in early school age and its influence on body posture. Brzek et al. BMC Musculoskeletal Disorders (2017) 18:117
https://bmcmusculoskeletdisord.biomedcentral.com/articles/10.1186/s12891-017-1462-z
Mitchell Roberts – Chiropractor
A few gardening tips!
Injuries from gardening is a common presentation to the clinic. We often fine with the changes in season, people come out to garden and do too much the first time after a long break.

Gardening is a lot of repetitive movements, of which if not done correctly, could lead to injury. A few tips on ensuring a comfortable gardening session:
- Warm up! Walk and a few stretches before you start will ensure your body is ready to start an active session
- Reduce the amount of twisting – Twisting places an uneven strain on the muscles and joints. Make sure you squarely face whatever you are working on, this minimises the amount of twisting that can occur.
- Take regular breaks! Especially if you are just starting gardening after a long time off. Frequent breaks are a great way to minimise injury and let the body rest and recover. Every 15-20 minutes with a 5-minute break in between is a good start.
- Keep your elbows bent when digging – this reduce the amount of strain on the forearm muscles. If they are over worked too quickly tennis elbow can occur – a form of tendinopathy.
- Frequently switch sides when raking those autumn leaves, keep the knees and elbows both bent and make sure your grip is relaxed. Also, using a scissor stance is the most efficient technique.
- Kneeling on one knee is the best position for weeding
- Use your hips and legs when picking up pots – stand square on bend at the hips and knees while keeping your back straight (think hinging at the hips). Keep the pot as close to your body as possible and avoid twisting while holding it.
- Plant pots on a table, not the ground
The most important thing to remember is to pace yourself!
Mitchell Roberts – Chiropractor